Big Benefits From Medicaid Expansion
Studies of 31 states extending Obamacare show better health and budget savings.

Former Health and Human Services Secretary Kathleen Sebelius and President Barack Obama. Official White House. Photo by Pete Souza.
There’s a rapidly growing body of academic research documenting the benefits of using the Affordable Care Act to expand Medicaid eligibility of adults.
Academic researchers love experiments with control groups, and those kinds of tests of public policy changes can be hard to find. However, the 2013 Supreme Court decision that made Medicaid expansions optional for states has been a boon for researchers. They can now study the changes in 31 states that have extended eligibility for adults to 138% of the poverty level, and can compare those states with the 19 “non-expansion” states. (Wisconsin is in the latter group because it caps BadgerCare eligibility for adults at the poverty level.)
One such study was published this month in the Journal of the American Medical Association Internal Medicine (JAMA). It compares health outcomes for patients in Kentucky and Arkansas – two states that accepted the expansion of Medicaid – with outcomes for patients in Texas, which has rejected it. The researchers found that the Medicaid expansion for low-income people in Kentucky and Arkansas was associated with increased access to primary care, fewer medications skipped due to cost, reductions in out-of-pocket spending and emergency department visits, and an increase in the share of adults reporting excellent health.
Shortly before that study came out, the Kaiser Family Foundation published a comprehensive review of 61 studies comparing expansion and non-expansion states. Collectively, these studies provide overwhelming evidence of the benefits of expanding Medicaid.
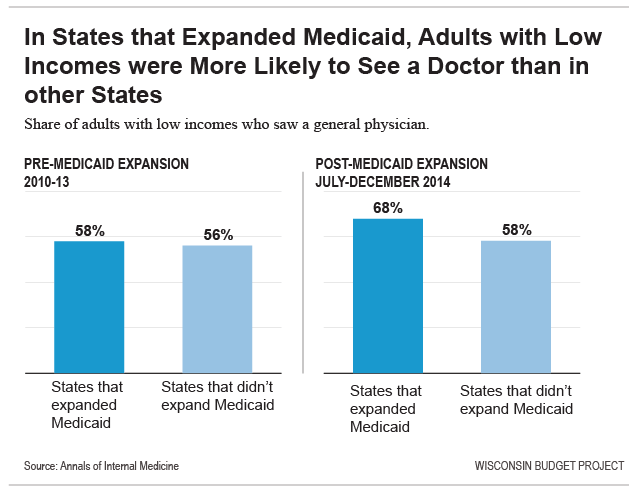
In States that Expanded Medicaid, Adults with Low Incomes were More Likely to See a Doctor than in other States
Here’s an overview of the findings, along with links to a number of the studies:
- Expansion states have enjoyed large coverage gains, including reductions in coverage disparities related to income and race.
- Medicaid expansion has been associated with positive impacts for low-income adults in terms of improved access to care and the utilization of services, including behavioral health services.
- The increased access and utilization of health care services is leading to increased diagnosis of chronic conditions, like diabetes.
- Expanding Medicaid has also been associated with improvements in the affordability of health care and has increased financial security for the expansion populations.
- Studies regarding the economic and fiscal impact of Medicaid expansion show that expansion states have seen budget savings and revenue gains, as well as reductions in uninsured hospital visits and uncompensated care costs.
The early survey data on insurance coverage show that Wisconsin has made some important gains since 2013, but not nearly as much as the Medicaid expansion states that cover all adults up to 138% of FPL. As a result, expanding BadgerCare to that level would yield the same types of benefits that have been seen in other states – in terms of increasing the insured rate, improving health, boosting financial security for families, and reducing the cost of uncompensated care that hospitals shift to their other patients.
Although the magnitude of those benefits would probably be smaller in Wisconsin, the fact that we are a partial expansion state means that we have even more to gain financially than other states from an eligibility expansion to 138% of FPL, since that would increase federal cost-sharing for many adults now covered by BadgerCare. According to a Legislative Fiscal Bureau memo, putting that change into effect by July of next year would save state taxpayers $392 million during the 2017-19 budget period, even though 82,000 more adults would be covered by BadgerCare.
In short, a rapidly growing body of research and the Fiscal Bureau memo show that a modest expansion of BadgerCare would be very positive for Wisconsin taxpayers, low-income families, and our health care system as a whole.
Wisconsin Budget
-
Charting The Racial Disparities In State’s Prisons
 Nov 28th, 2021 by Tamarine Cornelius
Nov 28th, 2021 by Tamarine Cornelius
-
State’s $1 Billion Tax Cut Leaves Out 49% of Taxpayers
 Sep 21st, 2021 by Tamarine Cornelius
Sep 21st, 2021 by Tamarine Cornelius
-
TANF Program Serves a Fraction of Poor Families
 Aug 30th, 2021 by Jon Peacock
Aug 30th, 2021 by Jon Peacock




















