Hundreds In Wisconsin Could Lose HIV Drug Help As State Trims Safety Net
DHS cost-cutting moves target an insurance-based program with a 95% viral suppression rate.
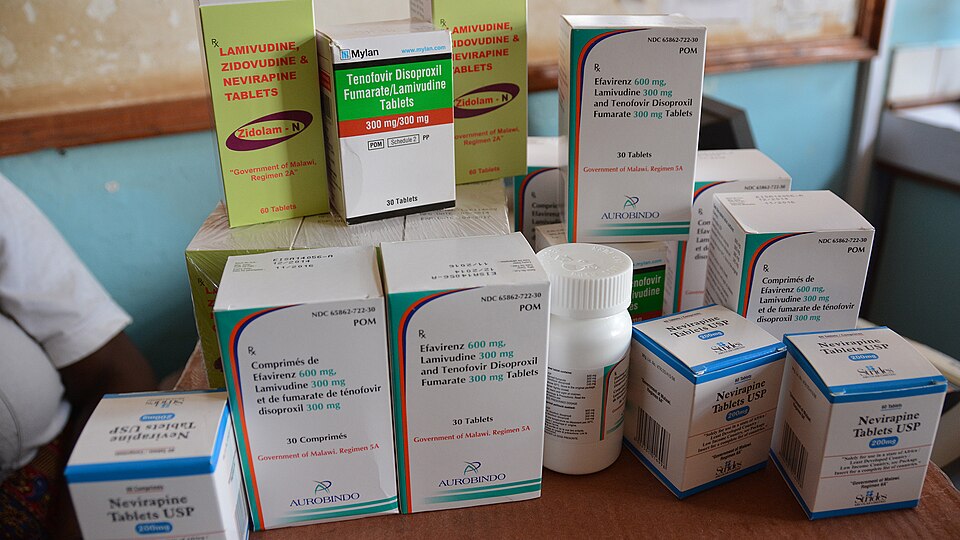
USAID in Africa, Public domain, via Wikimedia Commons
Every year, between 1,300 and 1,800 people with HIV in Wisconsin use a safety net program to purchase medications or access support services, according to state estimates from 2024. But recent cuts may jeopardize that option for hundreds of people across Wisconsin.
A recent analysis from the nonpartisan health policy organization KFF found that at least 18 states were enacting some form of restriction on their drug assistance programs for people with HIV/AIDS. The report argued that the measures could lead to these people losing access to care and treatment.
“States are facing fiscal pressures in many different directions,” Jen Kates, senior vice president at KFF, told WPR’s “Wisconsin Today.” “They are having to look at the different programs they support or the federal government supports and say, ‘What can we do to cut costs?’”
In a statement to WPR, the Wisconsin Department of Health Services confirmed instituting cost-cutting measures to the state’s HIV drug assistance program, writing that the cuts were done due to rising costs and increased enrollments.
“These were not easy decisions, but we found the actions to be necessary to continue to serve as many people as we can with the resources we have,” a spokesperson for the state DHS wrote.
The department confirmed that the state’s program will continue to cover the cost of HIV medications for clients without insurance and will cover premiums for nine types of insurance plans.
The state estimates around 400 people will be impacted — both by changes to the program that were made in January, as well as other changes set to take effect next year.
Wisconsin’s drug assistance
Wisconsin’s HIV Drug Assistance Program dates back to the passage of the Ryan White CARE Act in 1990. The largest component of the act provides grant money to state programs like Wisconsin’s.
These types of state-run safety net programs — called either HIV Drug Assistance Programs (HDAPs) or AIDS Drug Assistance Programs (ADAPs), depending on the state — provide assistance to people with HIV who live in households making at or below 300 percent of the federal poverty level.
The programs provide several types of assistance, including funding clinics for medical and support services to treat people with HIV, and purchasing HIV drugs outright for qualifying patients.
Wisconsin is trimming an aspect of the program Kates called innovative: the state’s practice of purchasing insurance plans for people with HIV.
“When you buy someone insurance, you’re not only giving them access to their medications but you’re giving them access to heart medication or any other health needs that they might have,” Kates said. “It’s really cost effective. It’s cheaper to buy health insurance for someone in the market than it is to buy just their medications.”
Kates said restrictions like this mean it will likely be harder for people with HIV to afford their medication, given rising costs tied to the expiration of the ACA Enhanced Tax Credits and cuts to Medicaid.
Doctor hails safety net program
Dr. Katherine Quinn is the Director of the Center for Community Health and Intervention Research at the Medical College of Wisconsin. For the last decade, she has studied how various social and structural factors influence HIV prevention, and whether treatment is successful.
One metric of success in treating HIV is whether a person is deemed “virally suppressed” — when the amount of HIV virus in someone’s blood has reduced to levels that are undetectable by a standard lab test. Quinn said 81 percent of people with HIV in Wisconsin are virally suppressed. But the state’s assistance program has a 95 percent success rate.
“This is a really incredible achievement that happens when people have access to HIV medications, when their insurance premiums are covered so that they don’t drop their plans, and when there are case managers available to help them navigate the system and show up when life gets really complicated,” Quinn said.
Quinn said the program’s approach to funding community agencies that assist with housing, mental health and substance use services are part of the reason for the high success rate.
“With the cuts in assistance to affording medications combined with the cuts to case management services, we could see a really large impact not just on the medication but also those social and structural factors that impact someone’s ability to adhere to their medications,” she said.
The Department of Health Services confirmed instituting funding cuts for medical and support services for agencies receiving a type of grant funding called Ryan White HIV/AIDS Program Part B funding. When WPR asked for specifics on the funding reduction and how many agencies would be impacted, the department declined to comment.
Quinn added there are few other options if people with HIV are cut from the state’s drug assistance program, as many childless adults with HIV aren’t eligible for BadgerCare or Medicaid and are left without affordable insurance alternatives.
These cuts may disproportionately affect Black and Hispanic people with HIV, she said, as they constitute a larger share of HDAP clients.
“They historically have faced some of the greatest barriers to health care,” Quinn said. “The fact that (Wisconsin’s) HDAP achieves 95 percent viral suppression across that population … is a genuine public health success story. These cuts are going to put that very vulnerable population at risk.”
Wisconsin is among at least 18 states cutting HIV safety net programs was originally published by Wisconsin Public Radio.
If you think stories like this are important, become a member of Urban Milwaukee and help support real, independent journalism. Plus you get some cool added benefits.