What Is The Future of Health Care?
Who’s gained the most from ACA and why Medicare for All could be a trap.
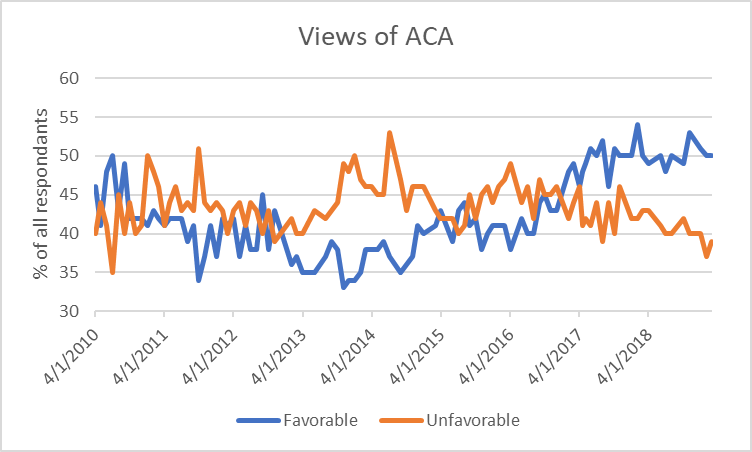
Following its passage—and particularly after its glitch-filled roll-out—the Affordable Care Act became deeply unpopular. The trick to its turnaround in public esteem seems to have been the election of Donald Trump, who seems intent on repealing the ACA without any clear vision of what, if anything, would replace it. The following plot shows the results of the Kaiser Family Foundation’s tracking poll since 2010, after passage of the ACA but before the implementation of its provisions. Since the spring of 2016, when its favorably rating was well below 40 percent, it has risen to as as high as a 54 percent favorable rating.
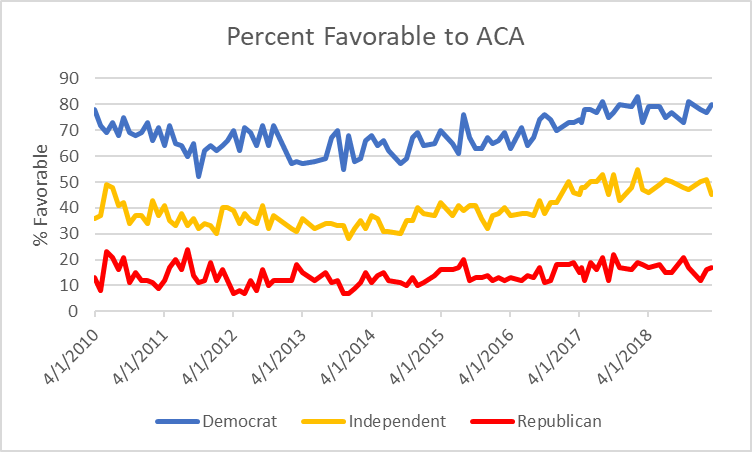
As the next graph shows, the improvement in the view of the ACA reflects greater favorability among Democrats (and, to a lesser extent, independents). Opinion among Republicans remains highly unfavorable to the ACA.
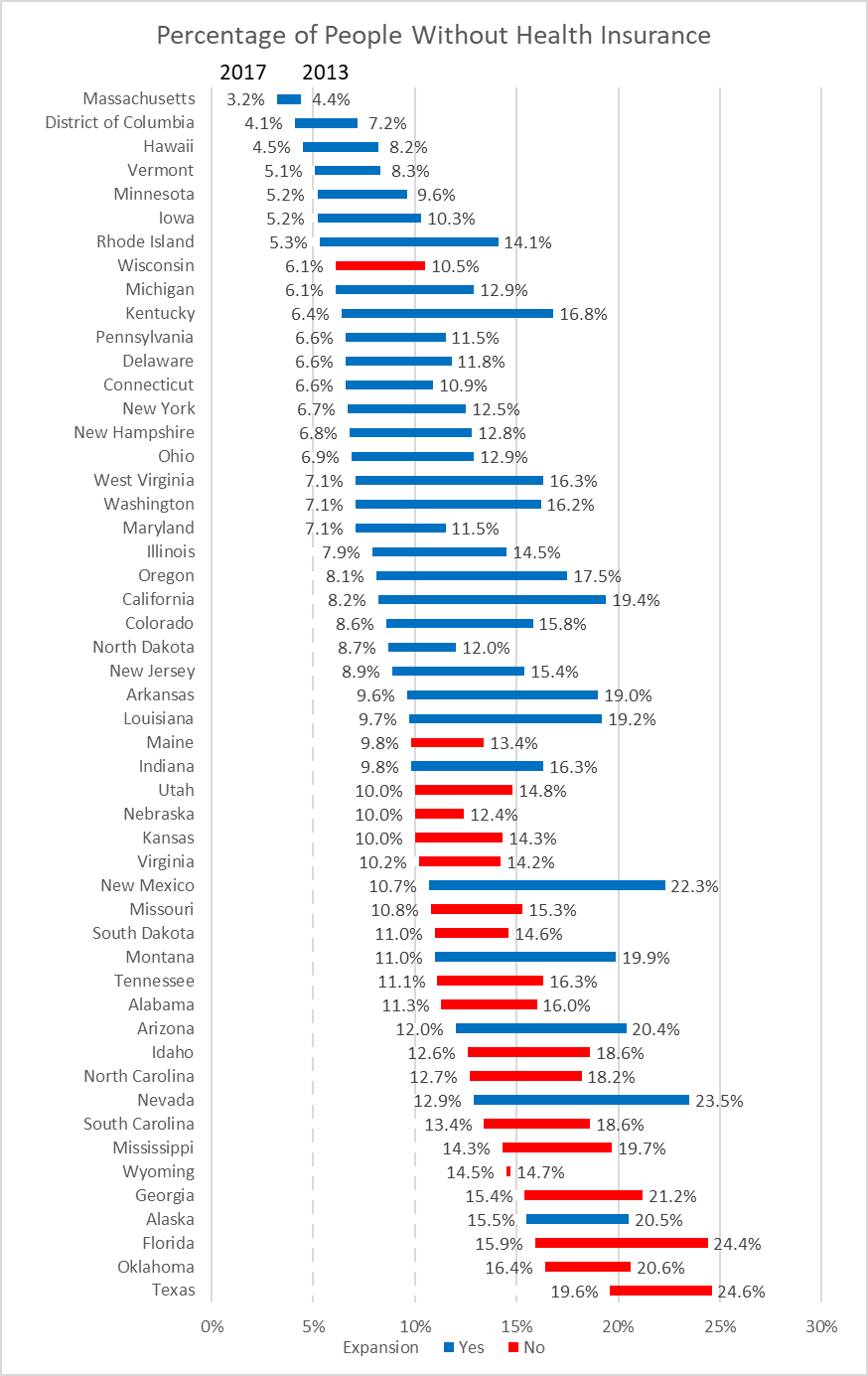
The next chart shows the percentage of people under age 65 without insurance by state in 2013 and 2017 based on the Kaiser Foundation’s analysis of US Census data. The right-hand side of each bar shows the uninsured in 2013, the last year before the ACA’s two major provisions—the expansion of Medicaid to cover everyone under 138 percent of the official poverty level and the introduction of the marketplace with its subsidies for those under 400 percent of the poverty level—took effect. The left side of the bars shows the percentage uninsured in 2017, the most recent year for which estimates are available. The decline in the percentage uninsured is shown in red if a state refused to expand Medicaid and blue if it did expand.
The graph above tells several stories. One is that the number of people without insurance is heavily dependent on a state’s Medicaid expansion decision. With the exception of Wisconsin, all the states in the top half accepted the offered federal subsidy to expand Medicaid.
Before the ACA, one-quarter of Texans had no health insurance, the worst of any state. By 2017 the number without insurance had dropped to one-fifth of the state’s population, 3 percent worse than Oklahoma, the next worse state.I find this puzzling: why would the leaders of Texas be proud of this record? And why would the former leaders of Wisconsin—Governor Scott Walker and Attorney General Brad Schimel—want Wisconsin to be associated with Texas in the lawsuit (Texas v. United States) to take away their constituents’ health insurance? Finally, why would they want to put Wisconsinites’ access to health insurance at risk by joining a lawsuit to end the ACA?
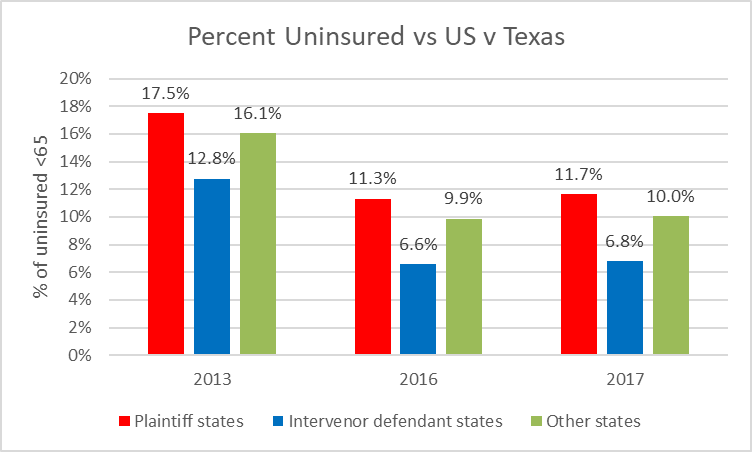
As the next chart shows, the worse a state’s pre-ACA record on insuring its residents, the more willing the state was to join the lawsuit to abolish the ACA’s coverage. The states suing to invalidate the ACA are shown in red, those intervening to protect the ACA in blue, and other states in green. For this chart, I removed Wisconsin from the plaintiffs.
Note that all three groups of states experienced a slight uptick in the number of uninsured in 2017, the first year of the Trump administration. Yet, despite the administration’s efforts to sabotage the ACA, the proportion of people without insurance in 2017 was slightly more than half that in 2013.
The ACA’s effect on health-care costs has received less attention. After comparing national health plans in the Netherlands, Switzerland, Canada, Australia, Germany, Norway, and England, Commonwealth Fund concluded that in 2016, “the United States spent nearly twice as much as 10 high-income countries on medical care and performed less well on many population health outcomes.” It concluded that “health care utilization in the United States did not differ substantially from other high-income nations. Prices of labor and goods, including pharmaceuticals and devices, and administrative costs appeared to be the main drivers of the differences in spending.”
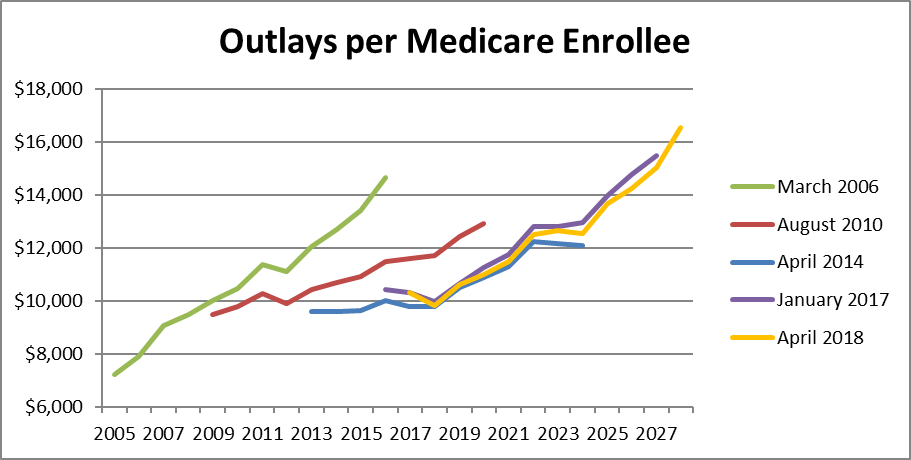
How did the ACA affect this problem? To prepare its budget estimates, the Congressional Budget Office must estimate future Medicare and other costs. The next chart compares several of these estimates. The green line shows the estimate from 2006, during the Bush administration. It estimated that the cost per enrollee would exceed $14,000 by 2016. The next line is from 2010, after the ACA was passed but before it was implemented. Future costs were both lower and rising slower than under the earlier estimate. The final three lines show estimates after implementation of the ACA. Costs per enrollee are projected to hit $14,000 a decade later than the 2006 estimate predicted.
Thus, in many ways, the ACA is a great success. Yet in coverage and costs it still falls short of plans in most other advanced countries. What should be done next?
One possibility is a single payer system, “Medicare-for-All,” supported by much of the Democratic base several of the candidates. If this involves ending employer-provided insurance, as some supporters insist, it may represent a trap for the Democrats.
It should be remembered that the unpopularity of the ACA during much of the Obama administration was not solely due to website glitches. Another factor was the promise that “if you like your plan, you can keep it.” It turned out that a lot of people liked the plans that the ACA banned. While the benefits were often lousy, the premiums were low.
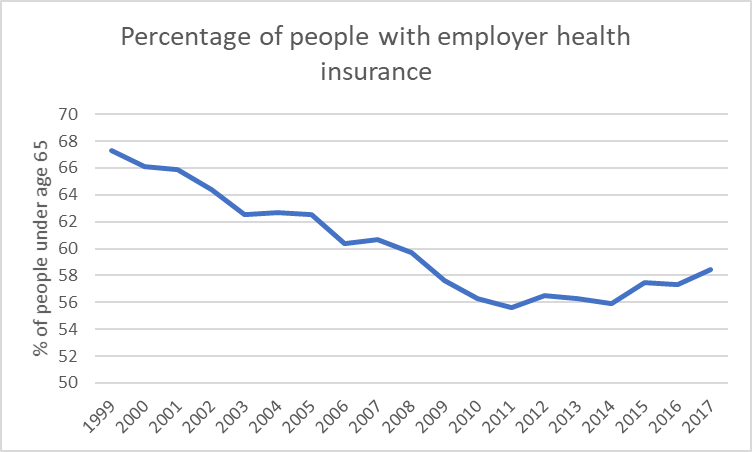
As the graph below demonstrates, employer-paid insurance has enjoyed a recent small uptick in enrollment, approaching 59 percent of people under 65. In addition, the ACA itself helps assure that these are good plans. For instance, there can no longer be lifetime caps on coverage.
A Kaiser poll in January found initial strong support for Medicare-for-All, but that support declined substantially when people were told that employer insurance policies would end. However, there is strong support for allowing people lacking employer insurance to buy into Medicare.
The 2018 election showed that protecting and expanding people’s access to health care insurance is a winning issue for Democrats. It is certainly helped along by Republican politicians’ strange fixation on taking away people’s insurance. However, Democrats risk losing their advantage if they allow Republicans to become the defenders of employer-based insurance.
Data Wonk
-
Who Do You Trust to Conduct Elections Fairly?
 Apr 6th, 2026 by Bruce Thompson
Apr 6th, 2026 by Bruce Thompson
-
Is Non-Citizen Voting a Real Threat to Elections in Wisconsin?
 Mar 18th, 2026 by Bruce Thompson
Mar 18th, 2026 by Bruce Thompson
-
How Global Climate Change Affects Milwaukee
 Mar 11th, 2026 by Bruce Thompson
Mar 11th, 2026 by Bruce Thompson























A few observations: First, and most important, there is a need to distinguish among three things: health insurance, health care and health. Bruce Thompson’s analysis is about health insurance. There are other critical discussions about the issues of cost, quality and accessibility of health care, and about the reality that there are large groups of unhealthy people and unhealthy communities in the Unites States.
The Affordable Care Act sought to address all of these issues in one way or another. It was based on the assumptions that it was essential to get everyone covered to address these problems, and that the current cost curve, especially for Medicare, was not sustainable, especially if aging people lived longer, but unhealthy lives.
The ACA was not unpopular because of the flawed rollout or other substantive reasons. It was unpopular because of the concerted effort of the Republican right and its allies to sabotage it right from the start, especially the dark money financiers and their corporate backers who sponsored the anti-ACA rallies and mobilized groups who believe that the only insurance and the only taxes that are worth paying for are ones that benefit them and screw everyone else.
As the old Republican lady in Florida said, “tell the government to keep its goddamn hands off my Medicare,” i.e., make sure no one else gets what I’ve got. That is the explanation for the willingness of the Republican states to screw their own citizens. Those being screwed are the surplus populations, mostly people who have been painted as the undeserving poor. They are also the groups that are most susceptible to chronic and environmental illnesses, conditions that will continue to deteriorate with our corporate controlled plutocracy and extraordinary inequality. Here, with respect to health insurance, is a fundamental question: should this vast sector be controlled by a handful of public companies that are driven by two things, shareholder value and executive compensation?
Finally, it was no secret that the ACA was imperfect, but there were fixes. For example, expanding coverage could have been achieved by increasing the fines for not being covered at the same time that the subsidies were also increased. It didn’t happened, and, possibly in the next couple of years, we will have TrumpCare, and the little old lady in Florida and lots of others who should have paid closer attention instead of looking for scapegoats are going to learn a harsh lesson.
Keep in mind the historical use of zoning ordinances to protect white middle and upper class neighborhoods from noxious industries and enterprises that attracted criminal behavior. Those elements were all concentrated in neighborhoods designated for communities of color, particularly African-American neighborhoods. With the advent of white suburbs, financed with federal support, we have the “supermarkets” with fresh foods available to middle class whites and food deserts in the inner cities and many rural communities. The pollution, crime, lack of nutritious food have created the health problems –asthma, diabetes, heart disease, mental illness and substance use disorders — of the “undeserving” poor predominantly communities of color. We have created our expensive, unsustainable, ineffective health system precisely because we label some as and others not deserving.